Diabetic Retinopathy
INTRODUCTION TO DIABETIC RETINOPATHY
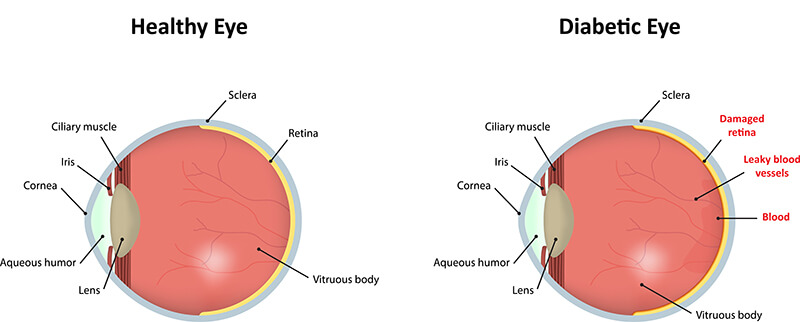
Major blood vessels lie on the front portion of the retina, and when these blood vessels are damaged due to diabetes, they may leak fluid and lipids (fats) and grow scar tissue. This leakage, called macular edema, affects the ability of the retina to detect and transmit images. Left unchecked, this may eventually lead to glaucoma, or cataracts, or a complete destruction of the retina, and even eventual blindness.
TYPES OF DIABETIC RETINOPATHY
There are two types of diabetic retinopathy:
- Nonproliferation diabetic retinopathy (NPDR)
- Proliferative diabetic retinopathy (PDR)
NONPROLIFERATION DIABETIC RETINOPATHY (NPDR)
Also known as background retinopathy, this is an early stage of diabetic retinopathy and occurs when the tiny blood vessels of the retina are damaged and begin to bleed or leak fluid into the retina resulting in swelling (diabetic macular edema) and the formation of deposits known as exudates. Many people with diabetes develop mild NPDR often without any visual symptoms.
PROLIFERATIVE DIABETIC RETINOPATHY (PDR)
This carries the greatest risk of loss of vision and typically develops in eyes with advanced NPDR. PDR occurs when blood vessels on the retina or optic nerve become blocked consequently starving the retina of necessary nutrients. In response, the retina grows more blood vessels (neovascularization). Unfortunately these new vessels are abnormal and cannot replenish the retina with normal blood flow. PDR may lead to any one of the following:
- Vitreous hemorrhage: proliferating retinal blood vessels grow into the vitreous cavity and break down. Both the hemorrhaging and resultant scar tissue may interfere with vision.
- Traditional retinal detachment: scar tissue in the vitreous and on the retina cause the retina to detach.
- Tractional and rhegmatogenous retinal detachment: scar tissue creates a hole or tear in the retina causing it to detach.
- Neovascular glaucoma: abnormal blood vessel growth on the iris blocks the flow of fluid out of the eye causing the pressure to increase and damaging the optic nerve.
SYMPTOMS OF DIABETIC RETINOPATHY
DIAGNOSTIC SIGNS OF DIABETIC RETINOPATHY
Things Dr. Seibel will look for and ask you about:- Changes in the blood vessels
- Retinal swelling (macular edema)
- Pale deposits on the retina
- Damaged nerve tissue
- Visual appearance of leaking blood vessels
- Dark floaters
- Loss of central or peripheral vision
- Visual distortions or blurriness
- Temporary or permanent vision loss
CAUSES OF DIABETIC RETINOPATHY
All people with diabetes are at risk – those with Type I diabetes (juvenile onset) and those with Type II diabetes (adult onset).
Although, everyone who has diabetes is at risk for developing diabetic retinopathy, not everyone develops it. Generally, diabetics don’t develop diabetic retinopathy until they’ve had diabetes for at least 10 years. Changes in blood sugar levels increase the risk.
Women with diabetes have a slightly higher risk during pregnancy. It is recommended that all pregnant women with diabetes have dilated eye examinations each trimester to protect their vision.
REDUCING THE RISK:
- Keep blood sugar under strict control
- Monitor blood pressure
- Maintain a healthy diet
- Exercise regularly
- Get an eye exam at least once a year
DIAGNOSING DIABETIC RETINOPATHY
A dilated eye exam is the only way to detect changes inside the eye before loss of vision begins. People with diabetes should have an eye examination at least once a year. More frequent exams may be necessary after diabetic retinopathy is diagnosed.
TESTS GIVEN FOR DETECTION
- Visual acuity test: The standard eye chart test is given to measure clarity of vision.
- Pupil dilation: Drops are placed into the eye to widen the pupil for a clear view of the retina. After the examination, close-up vision may remain blurred for several hours, and the patient will need dark glasses for sunlight and other bright lighting conditions.
- Ophthalmoscopy: This is an examination is done with two instruments:
- A handheld device with a bright light and a special magnifying lens provides a narrow magnified view of the retina
- A headset with a bright light and a special magnifying glass for a wide view of the retina
- Tonometry: A standard test that determines the fluid pressure inside the eye. Elevated pressure is a possible sign of glaucoma, more common in people with diabetes.
- Fluorescein angiography: This is a test for macular edema in which a harmless orange-red dye called fluorescein is injected into a vein in the arm. The dye travels to the blood vessels in the retina. A special camera, with a green filter, flashes a blue light into the eye and takes multiple photographs. The pictures will be analyzed to identify any damage to the lining of the retina or unusual blood vessels.
TREATMENT OF DIABETIC RETINOPATHY
Treatments are very effective in reducing vision loss from this disease. In fact, even people with advanced retinopathy have at least a 90 percent chance of keeping their vision if they get treatment before the retina is severely damaged. Treatments include:
- Laser treatments
- Vitrectomy
- Intraocular Medication
LASER TREATMENTS FOR DIABETIC RETINOPATHY
- Drops are administered to dilate your pupils and numb your eyes.
- In some cases, the area behind your eye may be numbed by injection as well to prevent any discomfort.
- A special lens is placed onto your eye.
- The lights in the office are dimmed. As you sit facing the laser, you may see flashes of light and notice a painless pinching sensation.
- Your pupils will remain dilated for a few hours, so you will need to wear dark wraparound sunglasses afterwards and arrange for someone to drive you home.
PROLIFERATIVE RETINOPATHY
A procedure called scatter laser treatment dissolves the abnormal blood vessels that form at the back of the eye. Rather than focusing on a single spot, hundreds of tiny laser zaps shrink the abnormal blood vessels from the center of the retina. Side vision is typically affected by this treatment in order to save the remaining central sight and may need repeating if new blood vessels appear.MACULAR EDEMA
This laser surgery, called focal laser treatment, if performed early enough can reduce vision loss from macular edema by half. During the surgery, a high-energy beam of light is aimed directly onto the damaged blood vessels. It seals the vessels and stops them from leaking. Sometimes, more than one treatment may be needed to completely control the leaking fluid.VITRECTOMY
Instead of laser surgery, an eye operation called a vitrectomy may be needed to restore sight. A vitrectomy is performed in cases that have a lot of blood in the vitreous. It involves removing the cloudy vitreous and replacing it with a special salt solution.- Studies show that people who have a vitrectomy soon after a large hemorrhage are more likely to protect their vision.
- Early vitrectomy is especially effective in people with insulin-dependent diabetes, who may be at greater risk of blindness from a hemorrhage into the eye.
- Vitrectomy is often done under local anesthesia, which means that you will be awake during the operation. Tiny incisions are made in the sclera, or white of the eye. Then, small instruments are placed into the eye that remove the vitreous and replace it with the salt solution.
- Your eye will be red and sensitive. You may be able to return home soon afterwards, or you may be asked to stay in the hospital overnight. An eye patch is required thereafter, for a few days or weeks to protect the eye, as well as medicated eye drops to protect against infection.